35,000
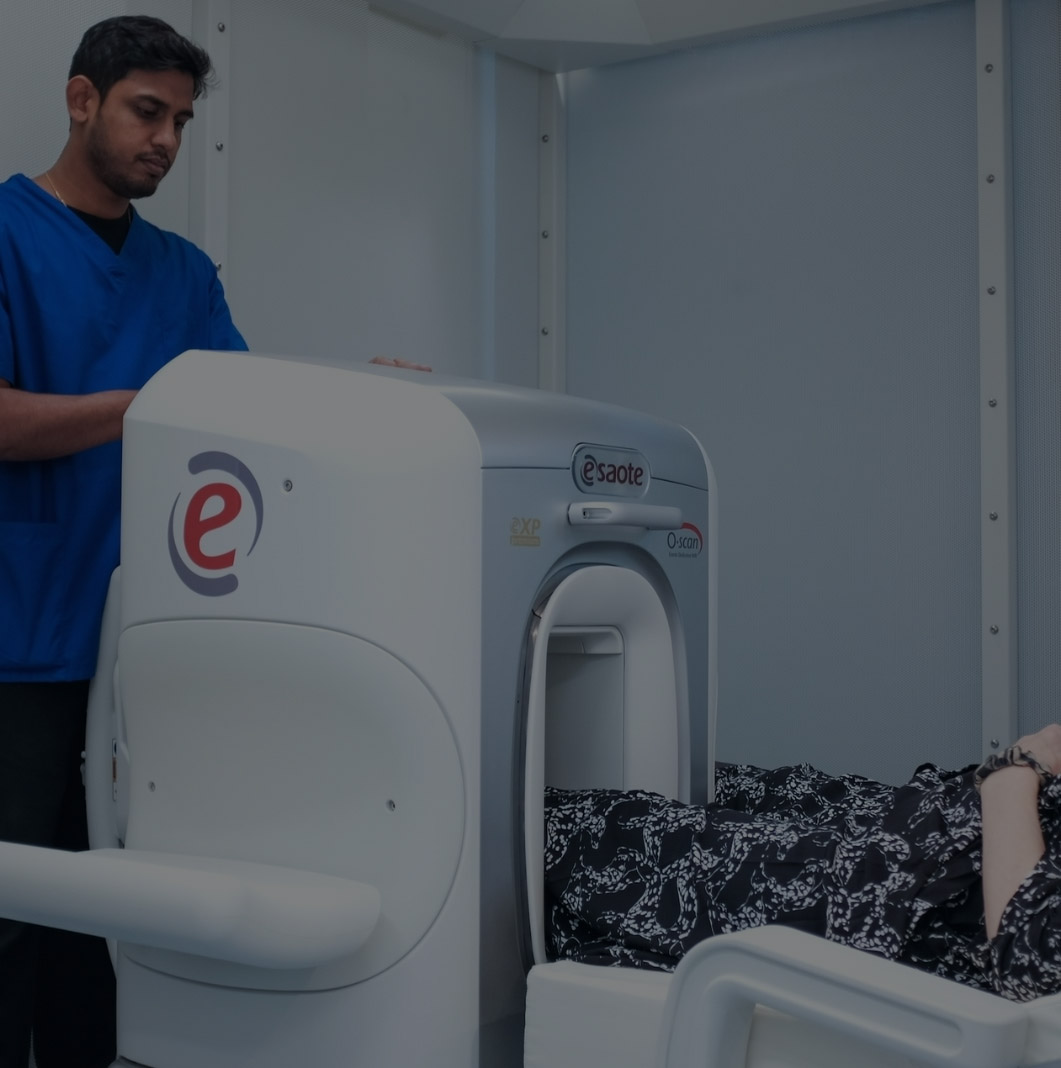
Lipogems® treatments
Lipogems® has been used in more than 35,000 patients worldwide.
2742
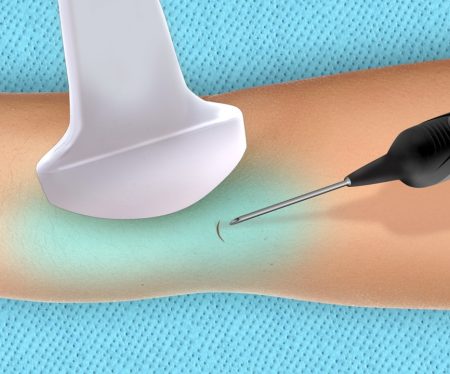
Joints Injected
As a clinic we have injected over 2700 joints with minimally invasive regenerative treatments
86%
Success Rate
Our results demonstrate that over 80% of patients have responded to their Lipogems® treatments
London
Clinic Location
All of our procedures are conducted in London. If you have recent x-ray or MRI results, we can offer a video consultation to anywhere in the world.
Treatments
Patient Stories
Our News
Read the latest developments and news in regenerative medicine
Meet Our Team
We have a team of leading surgeons and specialists who are global innovators in their own fields but also the most forward thinking in non-invasive, regenerative procedures.